- Air Sac Rupture
- Avian Influenza (Bird Flu)
- Bumblefoot
- Fowl cholera
- Poultry Rhinitis
- Fowlpox
- Histomoniasis (Blackhead disease)
- Avian Infectious Bronchitis
- Avian Infectious Laryngotracheitis (AILT)
- Coccidia
- Gapeworm
- Egg Binding
- Red Mite (Dermanyssus gallinae)
- Mycoplasmosis
- Marek’s Disease
- Newcastle Disease
- Ornithosis
- Salmonellosis
- Tuberculosis
- Vitamin B deficiency
- Worm Infestation
Air Sac Rupture
Symptoms
Air sac rupture is a condition that affects the respiratory system of birds, including turkeys. It occurs when one of the air sacs that help the bird breathe gets torn and allows air to escape under the skin. This causes a large balloon-shaped lump to form on the bird’s body, usually on the neck or head. The lump can vary in size and may grow very quickly. It may produce a crackling sound when touched and feel soft and spongy. The skin over the lump may look thin and transparent. The lump can interfere with the bird’s eating, breathing and movement, and may put pressure on internal organs.
Air sac rupture can be caused by various factors, such as trauma, infection, inflammation or congenital defects. The exact cause is often hard to determine. The diagnosis is usually based on the physical appearance of the lump and the history of the bird. A CT scan can be done to confirm the diagnosis if needed.
 Air Sac Rupture
(Picture by Lizzy Travis)
Treatment
The treatment for air sac rupture depends on the severity of the condition and the health of the bird. In some cases, the lump may heal by itself over time. In other cases, the lump may need to be punctured with a needle to release the air and reduce the swelling. This can be done by a veterinarian or by an experienced owner under veterinary guidance. The puncture site should be disinfected and monitored for infection. The bird should also be kept in a calm and comfortable environment and given supportive care.
Air sac rupture is a serious condition that can affect the quality of life and survival of turkeys. It is important to recognize the symptoms and seek veterinary attention as soon as possible.
Air Sac Rupture
(Picture by Lizzy Travis)
Treatment
The treatment for air sac rupture depends on the severity of the condition and the health of the bird. In some cases, the lump may heal by itself over time. In other cases, the lump may need to be punctured with a needle to release the air and reduce the swelling. This can be done by a veterinarian or by an experienced owner under veterinary guidance. The puncture site should be disinfected and monitored for infection. The bird should also be kept in a calm and comfortable environment and given supportive care.
Air sac rupture is a serious condition that can affect the quality of life and survival of turkeys. It is important to recognize the symptoms and seek veterinary attention as soon as possible.
Avian Influenza (Bird Flu)
Symptoms
The acute form of avian influenza manifests itself through general weakness (apathy, loss of appetite, dull, scrubby plumage), high fever, breathing difficulties with open beak, edema on the head, neck, crest, wattles, legs and feet, blue discoloration of the skin and the Mucous membranes, watery-slimy and greenish diarrhea and neurological disorders (strange posture of the head, motor disorders).
Under a chronic course, the laying performance decreases, the eggs have thin shells or are even shell-less.
Mortality depends on the age of the bird and the virulence of the pathogen. In the case of highly virulent pathogens, the disease is fatal in almost all animals. More than 15% of a flock of poultry can die before symptoms appear (peracute course).
Prevention
In principle, the animals could be effectively protected against avian influenza by a preventive vaccination. However, according to current knowledge, a live vaccine based on low pathogen pathogens is ruled out because of the risk of mutation. Immunization with inactivated influenza viruses is also controversial among experts, since no vaccine available to date prevents a later infection, the subsequent virus replication and the excretion of pathogenic viruses, rather only the clinical disease of the vaccinated animals is prevented. In this way, vaccinated animals can become virus carriers and spread pathogenic viruses. Another problem is the reliable (microbiological / serological) differentiation of the vaccinated animals from sick or contagious animals.
Treatment
In the event of outbreaks of avian influenza in animal husbandry, the entire animal population of the affected keeper is killed. The carcasses are burned or otherwise rendered harmless to prevent transmission to other livestock.
Symptoms
A bumblefoot is an infection of the foot (especially on the balls of the feet) that should not be underestimated and is caused by various causes. A bumblefoot can, if left untreated, lead to the death of an animal. Bacteria (e.g. staphylococci) penetrate the skin at the injured part of the foot and lead to a purulent abscess. If a bumblefoot is left untreated, it is very likely that the encapsulated infection on the turkey’s foot will spread first to the tendons, muscles and joints and finally to the entire organism. Then it becomes life-threatening for the animal, which is why early detection is important and immediate treatment is necessary.
 picture by Louise Humphreys
Prevention
Bumblefoot can be detected at an early stage by regular control of the feet, otherwise it will show up later in the form of mild or moderate lameness in the animal (protection of the affected foot). The bumble foot initially manifests itself swelling, scabs or a black point as the “entry point”. A good prophylaxis is clean underground, non-splintering perches and fine, soft bedding (e.g. hemp litter). A balanced, vitamin-rich feeding with grains, fresh fruit, vegetables, minerals and vitamins also contributes to the prevention. In addition, it is important to change the bedding regularly.
Treatment
First and foremost, it is always advisable to consult a poultry veterinarian in the case of a bumblefoot. In addition to the treatment (clearing out the purulent material and treating the wound), an antibiotic must be administered.
Important to know: The skin of the animal is very thick and leathery on the foot and the consistency of the pus, unlike humans, is extremely thick (similar to toothpaste). The affected foot of the animal must first be bathed in warm water with Betaisodona solution or similar. It is helpful to wrap the birds head in clothing during the treatment, so it can’t see anything, but can still breathe easily. First of all, the wound must be rinsed with Betaisodona solution or similar. Then an antiseptic ointment (e.g. Betaisodona ointment) in combination with Bepanthen creme for wound healing should be applied to the wound (please never ointment with a local anesthetic such as benzocaine, lidocaine or similar, as this is toxic for poultry, and can lead to death).
The wound should then be covered in a sterile manner and loosely connected with a sterile, elastic gauze bandage. As an intermediate layer, we recommend padding made of soft wadding to relieve pressure while walking. Finally, one protects against dirt and moisture self-adhesive bandage (blue or green – please not red, as the conspecifics feel encouraged to peck by the red color) as well as a layer of insulating tape under the bandage on the sole of the foot to protect against moisture. A wound check / bandage renewal is recommended every 2 days until completely healed. This can sometimes take 6-8 weeks, as the skin on the feet is slow heals and germs can penetrate the skin again at any time.
WikiHow: Link
picture by Louise Humphreys
Prevention
Bumblefoot can be detected at an early stage by regular control of the feet, otherwise it will show up later in the form of mild or moderate lameness in the animal (protection of the affected foot). The bumble foot initially manifests itself swelling, scabs or a black point as the “entry point”. A good prophylaxis is clean underground, non-splintering perches and fine, soft bedding (e.g. hemp litter). A balanced, vitamin-rich feeding with grains, fresh fruit, vegetables, minerals and vitamins also contributes to the prevention. In addition, it is important to change the bedding regularly.
Treatment
First and foremost, it is always advisable to consult a poultry veterinarian in the case of a bumblefoot. In addition to the treatment (clearing out the purulent material and treating the wound), an antibiotic must be administered.
Important to know: The skin of the animal is very thick and leathery on the foot and the consistency of the pus, unlike humans, is extremely thick (similar to toothpaste). The affected foot of the animal must first be bathed in warm water with Betaisodona solution or similar. It is helpful to wrap the birds head in clothing during the treatment, so it can’t see anything, but can still breathe easily. First of all, the wound must be rinsed with Betaisodona solution or similar. Then an antiseptic ointment (e.g. Betaisodona ointment) in combination with Bepanthen creme for wound healing should be applied to the wound (please never ointment with a local anesthetic such as benzocaine, lidocaine or similar, as this is toxic for poultry, and can lead to death).
The wound should then be covered in a sterile manner and loosely connected with a sterile, elastic gauze bandage. As an intermediate layer, we recommend padding made of soft wadding to relieve pressure while walking. Finally, one protects against dirt and moisture self-adhesive bandage (blue or green – please not red, as the conspecifics feel encouraged to peck by the red color) as well as a layer of insulating tape under the bandage on the sole of the foot to protect against moisture. A wound check / bandage renewal is recommended every 2 days until completely healed. This can sometimes take 6-8 weeks, as the skin on the feet is slow heals and germs can penetrate the skin again at any time.
WikiHow: Link
Fowl cholera
Symptoms
Fowl cholera can come in two forms.
• The peracute / acute form is characterized by septicemia, which in the peracute course is characterized by sudden death, acute fatigue, decreasing feed consumption, blue discolouration, shortness of breath and bloody nasal discharge and diarrhea. The morbidity in herds is up to 50%.
• The chronic form manifests itself in runny nose, inflammation of the head appendages (comb, wattles – “lobular disease”), joint inflammation, paralysis, torticollis, balance disorders and possibly diarrhea.
Prevention
The treatment of sick animals is usually unsuccessful. Therapy is therefore aimed at preventive antibiosis for endangered contact animals (metaphylaxis). Here sulfonamides or fluoroquinolones are used. Penicillins are also effective.
Treatment
Treatment of sick animals is usually unsuccessful (see prevention).
Poultry Rhinitis
Symptoms
• Inflamed eyes
• Nasal discharge
• Rattling breath noises
Prevention
• Barn hygiene
• Disinfection of automatic feeders and drinking troughs
• Avoidance of drafts in the stable
• Vitamin supplements
Fowlpox
Symptoms
After the second viraemia, the disease can manifest itself in different forms:
• The shape of the skin is characterized by papular changes, especially in non-feathered regions, around the eye, at the base of the beak, on the crest and on the posts. The papules dry up, turn yellowish and later brownish, and then fall off. If the course is mild, benign skin tumors often occur afterwards.
• The diphtheroid form is caused by fibrinous coatings on the mucous membranes in the beak and pharynx (oropharynx) and on the larynx. The diphtheroid form can be combined with skin symptoms.
• The septicemic form shows itself in general disorders such as fatigue, reluctance to eat and cyanosis. It usually ends fatally without the typical smallpox-like efflorescences occurring.
 Prevention
A live vaccine can be used for prophylaxis. This is given to animals that have not yet been infected, especially in the event of fowlpox outbreaks. Ornamental birds should be vaccinated at least in larger populations to protect them from fowlpox. The vaccine is given intramuscularly or by piercing the skin (wing-web method).
Treatment
Treatment is not possible.
Prevention
A live vaccine can be used for prophylaxis. This is given to animals that have not yet been infected, especially in the event of fowlpox outbreaks. Ornamental birds should be vaccinated at least in larger populations to protect them from fowlpox. The vaccine is given intramuscularly or by piercing the skin (wing-web method).
Treatment
Treatment is not possible.
Histomoniasis (Blackhead disease)
Symptoms
In turkeys in particular, histomoniasis leads to a severe course of the disease, with severe damage to the appendix and liver of the host.
The morbidity and mortality in infected birds is extremely high. The typical symptoms of histomoniasis are rather unspecific and infected animals show apathetic behavior, closed eyes, a stilted gait and breathing difficulties. In turkeys, the appearance of sulfur-yellow droppings as a result of liver damage is most noticeable, but in chickens it usually only results in slimy diarrhea. Liver lesions, however, do not occur.
However, histomoniasis can only be diagnosed with certainty after death. In turkeys, histomoniasis causes visible, necrotic lesions in the liver. In addition, there is a severe, ulcerative inflammation in the appendix of infected birds, which is associated with a characteristic thickening of the intestinal mucosa. Young animals usually die a few days after the onset of the disease; in older animals a chronic course is often observed. The disease takes its name from the blue-red to black discoloration of the scalp, which does not always occur. Since the appearance of black heads is not a primary indicator of histomoniasis, the term black head disease is sometimes viewed as a misnomer. Sometimes other organs can also be affected by histomoniasis.
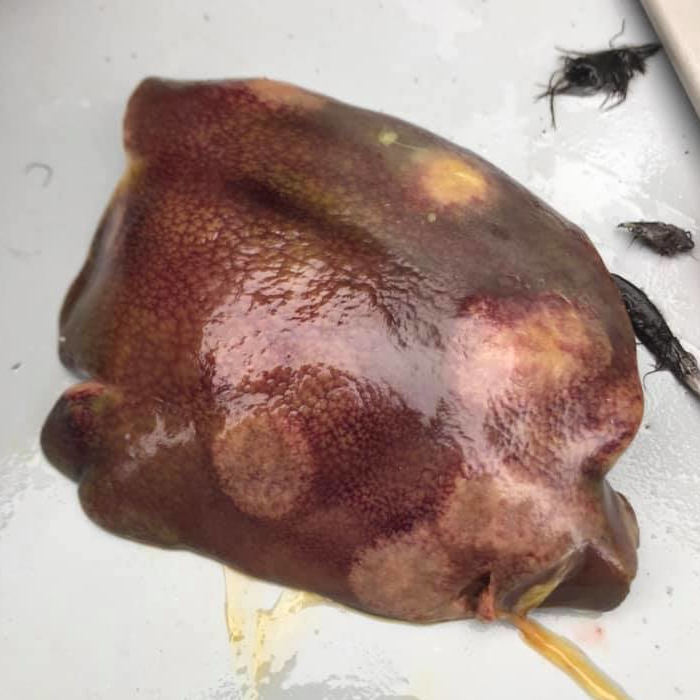 damaged liver by Blackhead disease
damaged liver by Blackhead disease
 healthy liver
healthy liver
 Sulfur-yellow poop due to Histomoniasis (picture by Michael Sagarese)
Prevention
Regular deworming of the animals has a prophylactic effect.
Treatment
Since the histomoniasis pathogen was identified, a large number of substances have been studied over time.
Various pentavalent arsenic compounds, such as nitarsone or carbasone, have proven to be effective in prophylactic use. In the European Union, they are no longer approved for food-producing animals. In the USA, however, nitarson (4-nitrophenyl arsenic acid) is still used.
Nifursol, which has a preventive effect, is no longer permitted today, just like other nitrofurans; The approval of Nifursol was revoked on April 1, 2003 across the EU.
Other active ingredients against the disease are Ronidazole and Dimetridazole, which are also no longer approved for poultry in the European Union.
Sulfur-yellow poop due to Histomoniasis (picture by Michael Sagarese)
Prevention
Regular deworming of the animals has a prophylactic effect.
Treatment
Since the histomoniasis pathogen was identified, a large number of substances have been studied over time.
Various pentavalent arsenic compounds, such as nitarsone or carbasone, have proven to be effective in prophylactic use. In the European Union, they are no longer approved for food-producing animals. In the USA, however, nitarson (4-nitrophenyl arsenic acid) is still used.
Nifursol, which has a preventive effect, is no longer permitted today, just like other nitrofurans; The approval of Nifursol was revoked on April 1, 2003 across the EU.
Other active ingredients against the disease are Ronidazole and Dimetridazole, which are also no longer approved for poultry in the European Union.
Avian Infectious Bronchitis
Symptoms
The transmission occurs primarily as a droplet infection, whereby grains of dust and droplets laden with viruses can travel long distances. The virus colonizes the ciliated epithelium of the airways, but the fallopian tubes can also be affected. IB spreads rapidly in a herd, especially young animals show a high incidence of the disease. The losses can be up to 25%.
The incubation time is 18 to 36 hours. Clinically, there are shortness of breath, nasal discharge, rattling breath noises and conjunctivitis. In addition, general disorders with unwillingness to eat can be observed. Fallopian tube infections later lead to laying disorders such as thin-shelled eggs, crab eggs, reduced or completely absent laying activity (“false layers”) and reduced hatching rate.
Prevention
Vaccination from the third week of life.
Treatment
The rapid spread in the population and the clinical manifestations allow a suspected diagnosis. The diagnosis can be made by pathological examination of dead birds as well as with serological and virological detection methods. Mycoplasmosis, infectious laryngotracheitis, chicken cold and Newcastle disease, as well as non-infectious diseases (feeding errors), must be differentiated.
Treatment is symptomatic at best. The control is therefore mainly based on the vaccination, which can be carried out from the third week of life. Repeat it every three to four months in endangered areas.
Avian Infectious Laryngotracheitis (AILT)
Symptoms
The pathogen causes mild to severe inflammation of the upper airways, mainly the larynx and windpipe (trachea). The disease occurs mainly in autumn and winter.
Clinically, it manifests itself in coughing, wheezing and shortness of breath, where the animals can choke out a bloody-colored mucus. Mild forms due to less virulent virus strains show up in sinusitis and conjunctivitis.
Pathological-anatomically, blood congestion and hyperemia of the larynx and trachea can be seen, if the course is severe, cheesy, diphtheroid coverings or pseudomembranes can appear, similar to the diphtheroid form of birdpox. In the epithelial cells, intranuclear inclusion bodies can be detected pathohistologically.
Prevention
see treatment
Treatment
The control is based on strict hygiene measures in poultry flocks to prevent the introduction of the pathogen. Vaccination with live vaccines is possible, but does not prevent latent infections or their flare-ups.
Coccidia
Symptoms
Coccidia is associated with bloody diarrhea and can have a mortality rate of 80% in chicks.
Prevention
Hygiene and disinfection measures can be used as a preventive measure. Boiling water is sufficient to inactivate the oocysts. Too high a stocking density is to be avoided, alternating outlets are recommended. In the event of an outbreak, the soil or litter should be removed. Effective disinfectants are z. B. Cresols. Chickens can be treated prophylactically with a coccidiostat. Vaccination of week-long chicks through the drinking water (Paracox 8®) is also effective.
Treatment
The treatment is carried out with drugs that act as coccidiostat, such as sulfonamides such as sulfachlorpyrazine or sulfadimidine. In addition, Toltrazuril and Clazuril are effective. Amprolium is very effective against coccidia. The administration of multivitamin preparations is recommended as a supplement.
Gapeworm
Symptoms
• Whistling or rattling breath noises
• Inflammation, swelling and small nodules at the attachment points, heavy mucus formation
• Moderate anemia
• Death from exhaustion or asphyxia
Prevention
Dry environment (prevents the formation of infectious larvae)
Treatment
Flubendazole
Egg Binding
Symptoms
A female bird that is affected by laying binding can initially be recognized by unsuccessful laying attempts. It tries to excrete the egg by pressing hard. Relatively large and thin balls of feces are excreted, which are often mixed with blood. Affected females appear nervous and restless, they often change seats, sit with widely spread legs on perches or see-saws with their tails. Pressure on nerve plexuses can lead to symptoms of paralysis.
At a later stage, affected females sit completely exhausted on the floor. Often a slight bulge can be noticed when touching the abdomen.
If not responded, the female will go into shock and die. Under certain circumstances, the strong pressing can lead to a cloaca prolapse.
Treatment
In the initial stage, an increase in the air humidity and heat radiation help. Furthermore, with the help of castor oil (or similar), which is trickled into the cloaca, an attempt can be made to loosen the egg. An abdominal massage (should only be used with larger birds, however, since the egg in the cloaca can break in small birds) in conjunction with the female’s attempts to press can help. If no success is achieved after a maximum of two hours, a veterinarian must be notified immediately. He can try to manually push the egg out of the cloaca, if this fails, the hormone oxytocin can be administered.
Red Mite (Dermanyssus gallinae)
Symptoms
The harmful effect of the red mite is caused by sucking blood, triggering itching and inflammation and the associated stress of the infected animals. Chicks and young birds can die due to the constant blood loss, even if the infestation is moderate. Direct deaths are also possible in broody birds.
Sick birds scratch their plumage irritably. There is inflammation and long-lasting itching at the bite sites. The mite infestation is particularly visible on the legs of the birds. In extreme cases, the skin here is severely swollen, crusted and flaky. Individual areas of the skin gradually peel off.
 Red Mite (De AW – Trabajo propio, CC BY-SA 2.5, https://commons.wikimedia.org/w/index.php?curid=6967126)
Prevention
A natural-based repellant can be used as an additive for the drinking water. This does not cause the mites to die off, but prevents the mites from sucking blood and thus interrupts the reproductive cycle.
Alternatively, a Fluralaner based solution can be used (e.g .: Exzolt (r) from MSD), which is also administered via the drinking water and actively kills the mites.
Treatment
The mites are typically controlled with acaricides in powder form (carbamates, pyrethroids, pyrethrum). Ivermectin has proven to be very effective.
The removal of the mites from roosters is more problematic. Here all hiding places must be thoroughly cleaned and treated with acaricides. Alternatively, a 2-component disinfectant based on peroxyacetic acid and hydrogen peroxide can be used.
An alternative to acaricides are silicate dust (kieselguhr). The mode of action is based on a drying effect on contact. Another option is to coat the underside of the perches with vegetable oil (basically all oils). Here the oil clogs the pores and suffocates all stages of the mites.
Red Mite (De AW – Trabajo propio, CC BY-SA 2.5, https://commons.wikimedia.org/w/index.php?curid=6967126)
Prevention
A natural-based repellant can be used as an additive for the drinking water. This does not cause the mites to die off, but prevents the mites from sucking blood and thus interrupts the reproductive cycle.
Alternatively, a Fluralaner based solution can be used (e.g .: Exzolt (r) from MSD), which is also administered via the drinking water and actively kills the mites.
Treatment
The mites are typically controlled with acaricides in powder form (carbamates, pyrethroids, pyrethrum). Ivermectin has proven to be very effective.
The removal of the mites from roosters is more problematic. Here all hiding places must be thoroughly cleaned and treated with acaricides. Alternatively, a 2-component disinfectant based on peroxyacetic acid and hydrogen peroxide can be used.
An alternative to acaricides are silicate dust (kieselguhr). The mode of action is based on a drying effect on contact. Another option is to coat the underside of the perches with vegetable oil (basically all oils). Here the oil clogs the pores and suffocates all stages of the mites.
Mycoplasmosis
Symptoms
The disease (mycoplasmosis) usually manifests itself as an initially dry, short sneeze that is expelled through the nostrils with the beak closed. With a progressive spread in the respiratory tract, clear discharge from the nostrils can also be seen in the form of a moist film towards the tip of the beak. This film is particularly noticeable when leftover food and litter stick around the openings.
 Treatment
A rehabilitation of the affected population is only possible by interrupting the chain of infection. Mycoplasma gallisepticum reacts to the antibiotic tylosin. The symptoms can thus be suppressed for a short time, but reinfection takes place promptly if the stall is full, as the bacterium outside the body in the environment (stall, exercise area) maintains its ability to infect for a limited time. The occurrence of symptoms facilitates infection by other economically important respiratory diseases such as B. Infectious Bronchitis (IB) and Avian Rhinotracheitis (ART).
Treatment
A rehabilitation of the affected population is only possible by interrupting the chain of infection. Mycoplasma gallisepticum reacts to the antibiotic tylosin. The symptoms can thus be suppressed for a short time, but reinfection takes place promptly if the stall is full, as the bacterium outside the body in the environment (stall, exercise area) maintains its ability to infect for a limited time. The occurrence of symptoms facilitates infection by other economically important respiratory diseases such as B. Infectious Bronchitis (IB) and Avian Rhinotracheitis (ART).
Marek’s Disease
Symptoms
The incubation period is 20 to 160 days. Marek’s disease is very variable in its clinical picture.
In the classic form, the colonization of the nerves dominates and paralysis occurs in animals aged between 12 and 16 weeks. It occurs sporadically and the mortality is below 10%.
The acute form is epidemic in chicks up to the 8th week of life and leads to deaths especially in 18–22 week old animals. There can also be late deaths at the beginning of the first laying period. The mortality rate is up to 50%. The acute form shows up in bumps in the skin that lead to rough skin, as well as lymphomas in the bowels.
Prevention
Vaccination on the first day of life.
A treatment is not possible, which is why control focuses on prevention. It takes place through veterinary hygiene measures. Vaccination on the first day of life is possible, but is only carried out in breeding animals and laying hens. The breeding of resistant chickens is also being tried.
Newcastle Disease
Symptoms
The clinical picture of Newcastle disease initially shows numerous unspecific changes in the behavior and appearance of the animals, as they also occur with other acute infections:
• Drastic drop in egg production and thin-shelled to shell-less eggs
• High fever of up to 43 ° C
• Apathy and loss of appetite
• Watery, possibly bloody diarrhea
• Shortness of breath; The beak and eyes are covered with thick mucus
• Circulatory disorders, often with dark crest discoloration
• High mortality within five days of the onset of the symptoms
The incubation period is four to six days. If it spreads rapidly within the herd, deaths can also occur without any previously recognizable symptoms.
The viruses attack the lungs, intestines and central nervous system and can, among other things, cause punctiform bleeding on the lining of the stomach, especially around the ducts of the gastric glands.
In rare cases, inflammation of the conjunctiva of the eye can occur in people who are in close contact with sick animals.
Prevention
Regular vaccination against Newcastle disease for every flock of chickens and turkeys. The vaccination is usually done through the drinking water.
Treatment
Infected animals must be killed immediately. Affected stables, buildings and transport vehicles must be disinfected. Additional restrictions on people and traffic may be imposed on the keeping of animals.
Ornithosis
Symptoms
This severe, flu-like general illness usually progresses with predominant involvement of the lungs (bronchopneumonia).
Treatment
As a rule, antibiotic therapy with tetracyclines (such as tetracycline, doxycycline) or macrolides (such as clarithromycin, erythromycin) takes two to three weeks.
Salmonellosis
Symptoms
Salmonellosis in chickens: S. gallinarum is adapted to chickens, but can also occur in turkeys and some other bird species. This serovar occurs in 2 biovars: Biovar pullorum is responsible for the white chick dysentery or pullorum disease and leads to acute septicemic infections in chicks up to the 3rd to 6th week of life. The Biovar Gallinarum is the cause of so-called chicken typhus, which occurs mainly in older chickens. Infections with non-adapted types usually do not cause disease in chickens, but latent infections.
Prevention
Vaccination of all those who are still healthy with a live vaccine.
Treatment
• Eliminate all sick animals
• Treatment of the population with antibiotics
Tuberculosis
Symptoms
As in cattle and humans, the various organ systems in birds are affected.
Treatment
Treatment of animals must not be carried out because the risk of infection for humans during or after the treatment due to resistant germs or chronically germ-releasing animals. In humans, special antibiotics must be used intensively over a long period of time.
Vitamin B deficiency
Symptoms
Neurological disorders, symptoms of paralysis, convulsions;
Prevention
• Vitamin supplements
• Food additives
Treatment
Vitamin supplements
Food additives
Worm Infestation
Symptoms
Chickens and turkeys are very susceptible to parasitic worms. These include the tracheal worms, the tapeworms and the roundworms. While not all types of worms are harmful to the health system, some can lead to weight loss, poor egg production, and even death.
Prevention
Regularly deworming
Treatment
The use of drugs to combat worms (anthelmintics) is particularly important in the field of veterinary medicine. The most important class of substances at the moment are the benzimidazoles, the most widely used representatives of which, in addition to flubendazole, are primarily fenbendazole and mebendazole. Also frequently used groups of active substances are tetrahydropyrimidines (here especially the pyrantel) and imidazothiazoles (especially levamisole). Ivermectins (e.g. moxidectin, doramectin, milbemycin) are considered to be a relatively new group of active ingredients. Older anthelmintics such as piperazine or organic phosphoric acid esters such as dichlorvos only play a subordinate role.
Air Sac Rupture (Picture by Lizzy Travis) Treatment The treatment for air sac rupture depends on the severity of the condition and the health of the bird. In some cases, the lump may heal by itself over time. In other cases, the lump may need to be punctured with a needle to release the air and reduce the swelling. This can be done by a veterinarian or by an experienced owner under veterinary guidance. The puncture site should be disinfected and monitored for infection. The bird should also be kept in a calm and comfortable environment and given supportive care. Air sac rupture is a serious condition that can affect the quality of life and survival of turkeys. It is important to recognize the symptoms and seek veterinary attention as soon as possible.
picture by Louise Humphreys Prevention Bumblefoot can be detected at an early stage by regular control of the feet, otherwise it will show up later in the form of mild or moderate lameness in the animal (protection of the affected foot). The bumble foot initially manifests itself swelling, scabs or a black point as the “entry point”. A good prophylaxis is clean underground, non-splintering perches and fine, soft bedding (e.g. hemp litter). A balanced, vitamin-rich feeding with grains, fresh fruit, vegetables, minerals and vitamins also contributes to the prevention. In addition, it is important to change the bedding regularly. Treatment First and foremost, it is always advisable to consult a poultry veterinarian in the case of a bumblefoot. In addition to the treatment (clearing out the purulent material and treating the wound), an antibiotic must be administered. Important to know: The skin of the animal is very thick and leathery on the foot and the consistency of the pus, unlike humans, is extremely thick (similar to toothpaste). The affected foot of the animal must first be bathed in warm water with Betaisodona solution or similar. It is helpful to wrap the birds head in clothing during the treatment, so it can’t see anything, but can still breathe easily. First of all, the wound must be rinsed with Betaisodona solution or similar. Then an antiseptic ointment (e.g. Betaisodona ointment) in combination with Bepanthen creme for wound healing should be applied to the wound (please never ointment with a local anesthetic such as benzocaine, lidocaine or similar, as this is toxic for poultry, and can lead to death). The wound should then be covered in a sterile manner and loosely connected with a sterile, elastic gauze bandage. As an intermediate layer, we recommend padding made of soft wadding to relieve pressure while walking. Finally, one protects against dirt and moisture self-adhesive bandage (blue or green – please not red, as the conspecifics feel encouraged to peck by the red color) as well as a layer of insulating tape under the bandage on the sole of the foot to protect against moisture. A wound check / bandage renewal is recommended every 2 days until completely healed. This can sometimes take 6-8 weeks, as the skin on the feet is slow heals and germs can penetrate the skin again at any time. WikiHow: Link
Prevention A live vaccine can be used for prophylaxis. This is given to animals that have not yet been infected, especially in the event of fowlpox outbreaks. Ornamental birds should be vaccinated at least in larger populations to protect them from fowlpox. The vaccine is given intramuscularly or by piercing the skin (wing-web method). Treatment Treatment is not possible.
damaged liver by Blackhead disease
healthy liver
Sulfur-yellow poop due to Histomoniasis (picture by Michael Sagarese) Prevention Regular deworming of the animals has a prophylactic effect. Treatment Since the histomoniasis pathogen was identified, a large number of substances have been studied over time. Various pentavalent arsenic compounds, such as nitarsone or carbasone, have proven to be effective in prophylactic use. In the European Union, they are no longer approved for food-producing animals. In the USA, however, nitarson (4-nitrophenyl arsenic acid) is still used. Nifursol, which has a preventive effect, is no longer permitted today, just like other nitrofurans; The approval of Nifursol was revoked on April 1, 2003 across the EU. Other active ingredients against the disease are Ronidazole and Dimetridazole, which are also no longer approved for poultry in the European Union.
Red Mite (De AW – Trabajo propio, CC BY-SA 2.5, https://commons.wikimedia.org/w/index.php?curid=6967126) Prevention A natural-based repellant can be used as an additive for the drinking water. This does not cause the mites to die off, but prevents the mites from sucking blood and thus interrupts the reproductive cycle. Alternatively, a Fluralaner based solution can be used (e.g .: Exzolt (r) from MSD), which is also administered via the drinking water and actively kills the mites. Treatment The mites are typically controlled with acaricides in powder form (carbamates, pyrethroids, pyrethrum). Ivermectin has proven to be very effective. The removal of the mites from roosters is more problematic. Here all hiding places must be thoroughly cleaned and treated with acaricides. Alternatively, a 2-component disinfectant based on peroxyacetic acid and hydrogen peroxide can be used. An alternative to acaricides are silicate dust (kieselguhr). The mode of action is based on a drying effect on contact. Another option is to coat the underside of the perches with vegetable oil (basically all oils). Here the oil clogs the pores and suffocates all stages of the mites.
Treatment A rehabilitation of the affected population is only possible by interrupting the chain of infection. Mycoplasma gallisepticum reacts to the antibiotic tylosin. The symptoms can thus be suppressed for a short time, but reinfection takes place promptly if the stall is full, as the bacterium outside the body in the environment (stall, exercise area) maintains its ability to infect for a limited time. The occurrence of symptoms facilitates infection by other economically important respiratory diseases such as B. Infectious Bronchitis (IB) and Avian Rhinotracheitis (ART).
